SVT (supraventricular tachycardia)
SVT (supraventricular tachycardia)
Diagnostic criteria: (boldfaced with * indicates an important feature)- * Rate: > 100, but typically > 150
- Rhythm: regular
- * P waves: not easily identified (but they could be present)
- * PR interval: no P waves identified
- QRS: narrow
Electrophysiology
SVT is an "umbrella" term that means any tachycardia that is NOT ventricular tachycardia. Any of the following rhythms could be classified as SVT:- sinus tachycardia
- atrial tachycardia
- atrial flutter
- atrial fibrillation (if it looks quite regular as opposed to having an irregular rhythm)
- AV node re-entry tachycardia (AVNRT)
- Atrio-Ventricular re-entry tachycardia (AVRT) (this rhythm requires an accessory pathway, such as WPW)
There are a few more items that could go into this list, but this list covers > 95% of all SVT.
When the ventricular rate is very high, the space between QRS's is very short. In this very short space, there is a T wave and MAYBE a P wave. However, because of the high frequency of QRS complexes, it is very difficult to determine which waveforms are present in this very short space. Therefore, to make our lives simpler, we classify these very fast NARROW QRS COMPLEX tachycardia's as SVT.
"Wide QRS complex" tachycardia would be the "other category" of tachycardia (see also the next lesson on ventricular tachycardia and the separate module on Bundle Branch Blocks). There are 2 common causes (and a few not so common causes) of wide complex tachycardia:- ventricular tachycardia (VT)
- any SVT in combination with an abnormal conduction system in the ventricles, such as bundle branch block. These rhythms are called SVT "with abberancy".
It is important to compare and contrast SVT vs. VT:- Differences:
- SVT is a narrow QRS and VT is a wide QRS
- SVT originates from either the SA node, atria or AV node, while VT always originates from the ventricle
- VT is more dangerous than SVT
- Similarities:
- both rhythms are very fast
- P waves are usually NOT seen in both rhythms
Clinical Significance:
The most important detail for clinical significance is the heart rate. The higher the heart rate is, the worse the patient will be. The reason why inapropriate high heart rates are bad is that filling time for each heart beat is reduced. The amount of time that the heart spends in diastole is the time for ventricular filling.
Let's do a math example: a heart rate of 240 will result in 4 heartbeats per second. This means that each cardiac cycle lasts 0.25 seconds (a quarter of a second). If we assume that systole and diastole each occupy 50% of the cardiac cycle, then there is 0.125 second (one eighth of a second) for the heart to fill. This is not enough time to fill the ventricle and the stroke volume, cardiac output, and blood pressure will all be very low.
SVT can be treated with some drugs, or if severe and non-responsive to drugs, can be treated with cardioversion. Cardioversion is similar to defibrillation in that both administer a very large shock to the patient. The difference is that cardioversion is "timed" with the ECG so that the electric shock does not land of the T wave (this can precipiate ventricular fibrillation).
There is an "SVT" algorithm in ACLS (Advanced Cardiac Life Support) which is a course that teaches how to resuscitate patients in cardiac arrest.
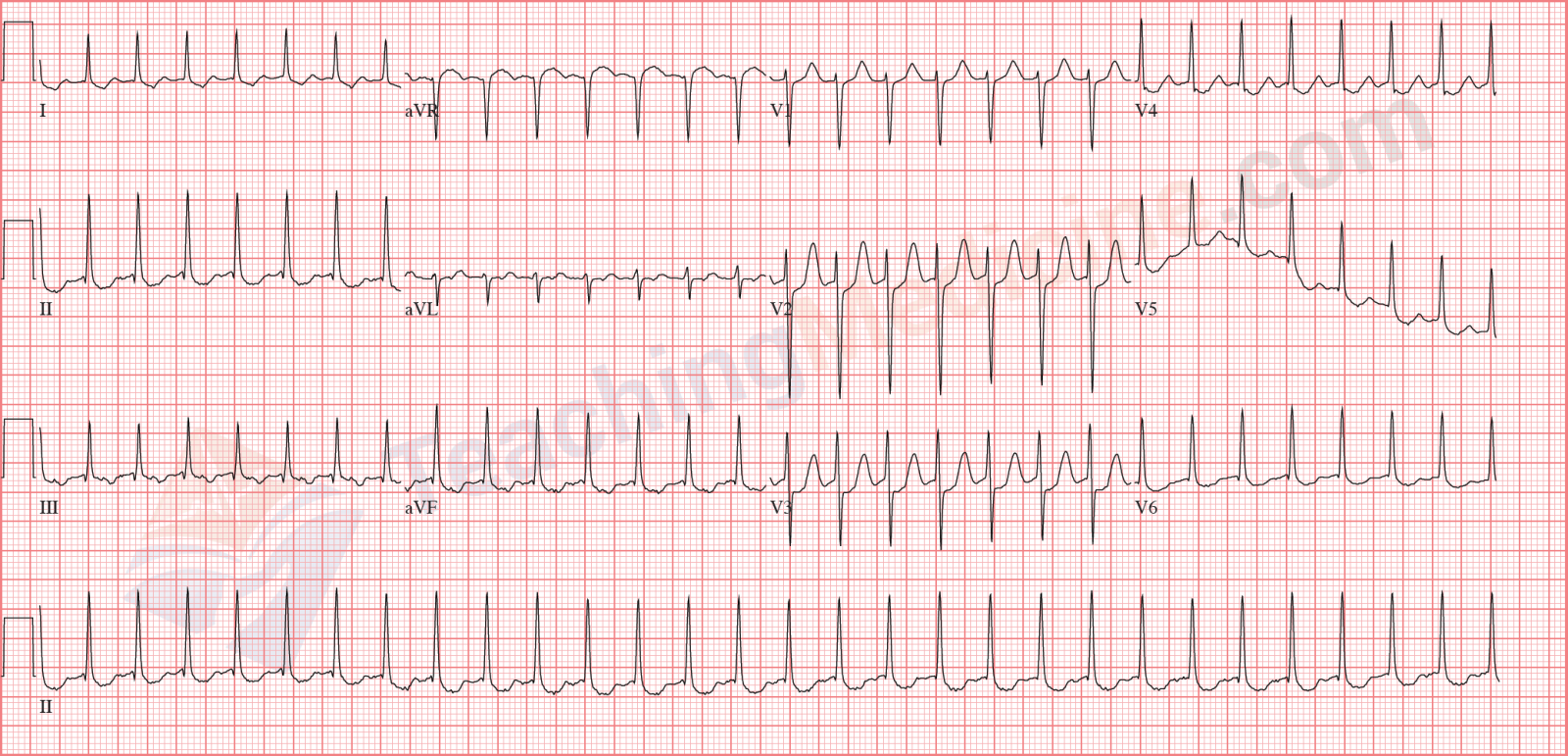
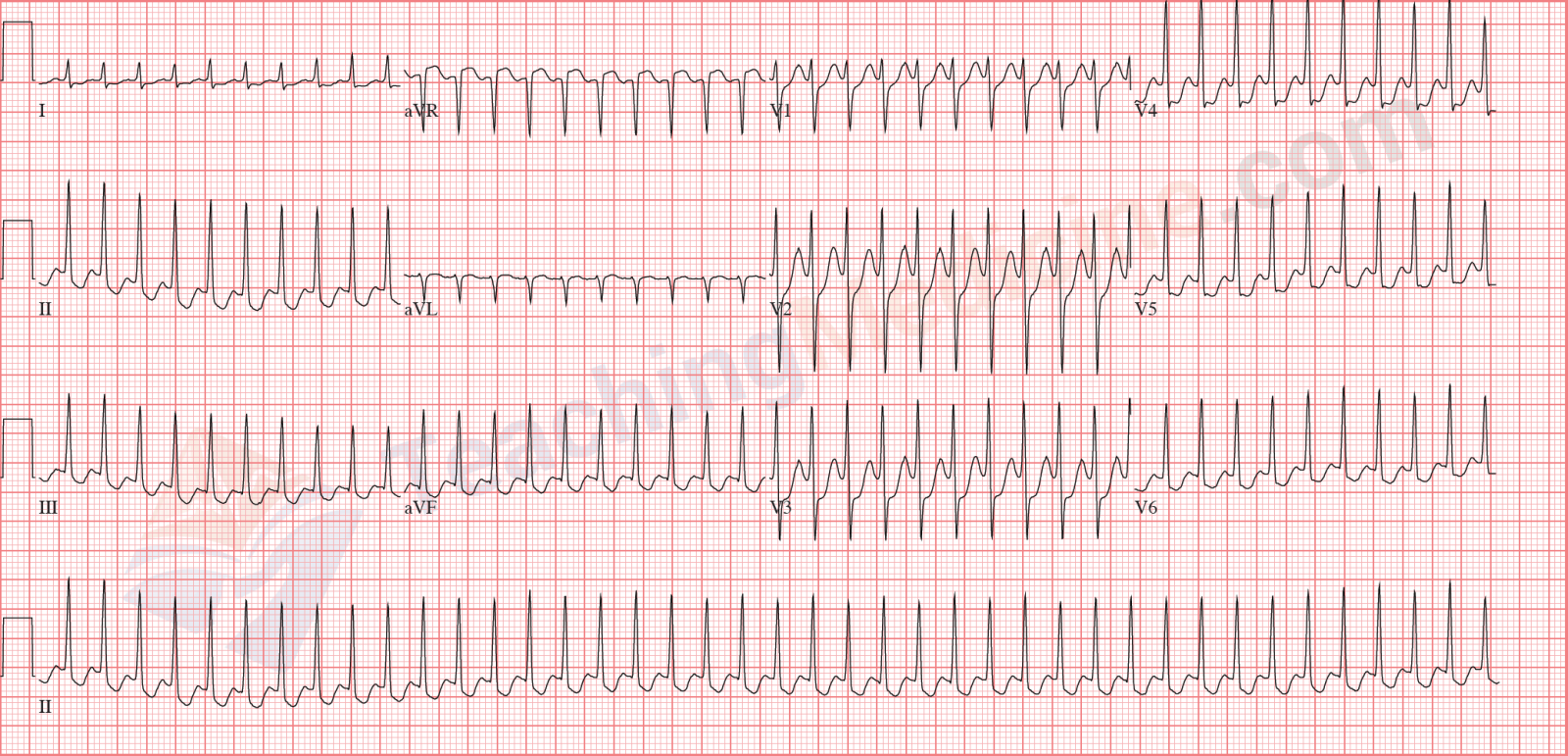
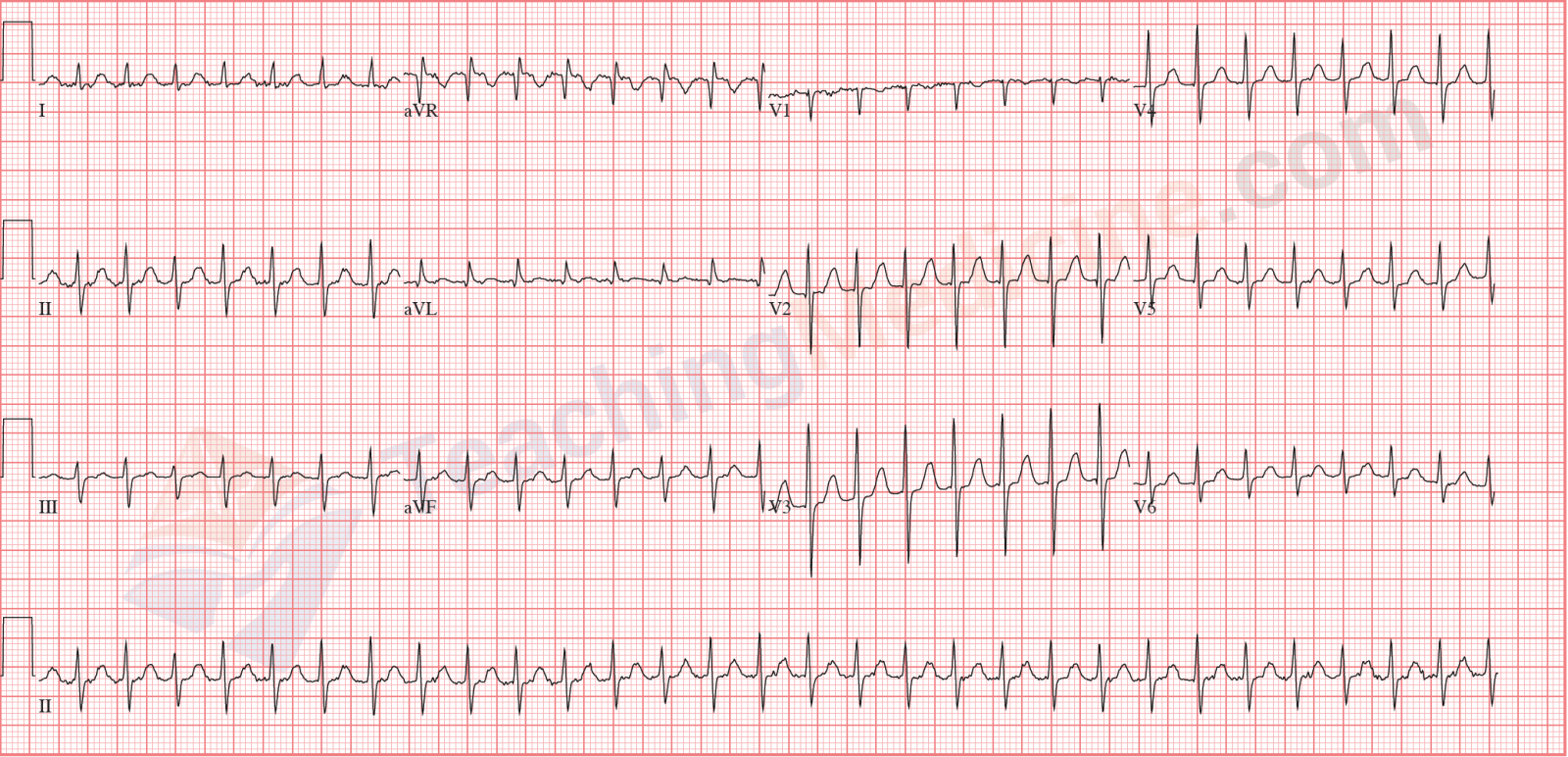
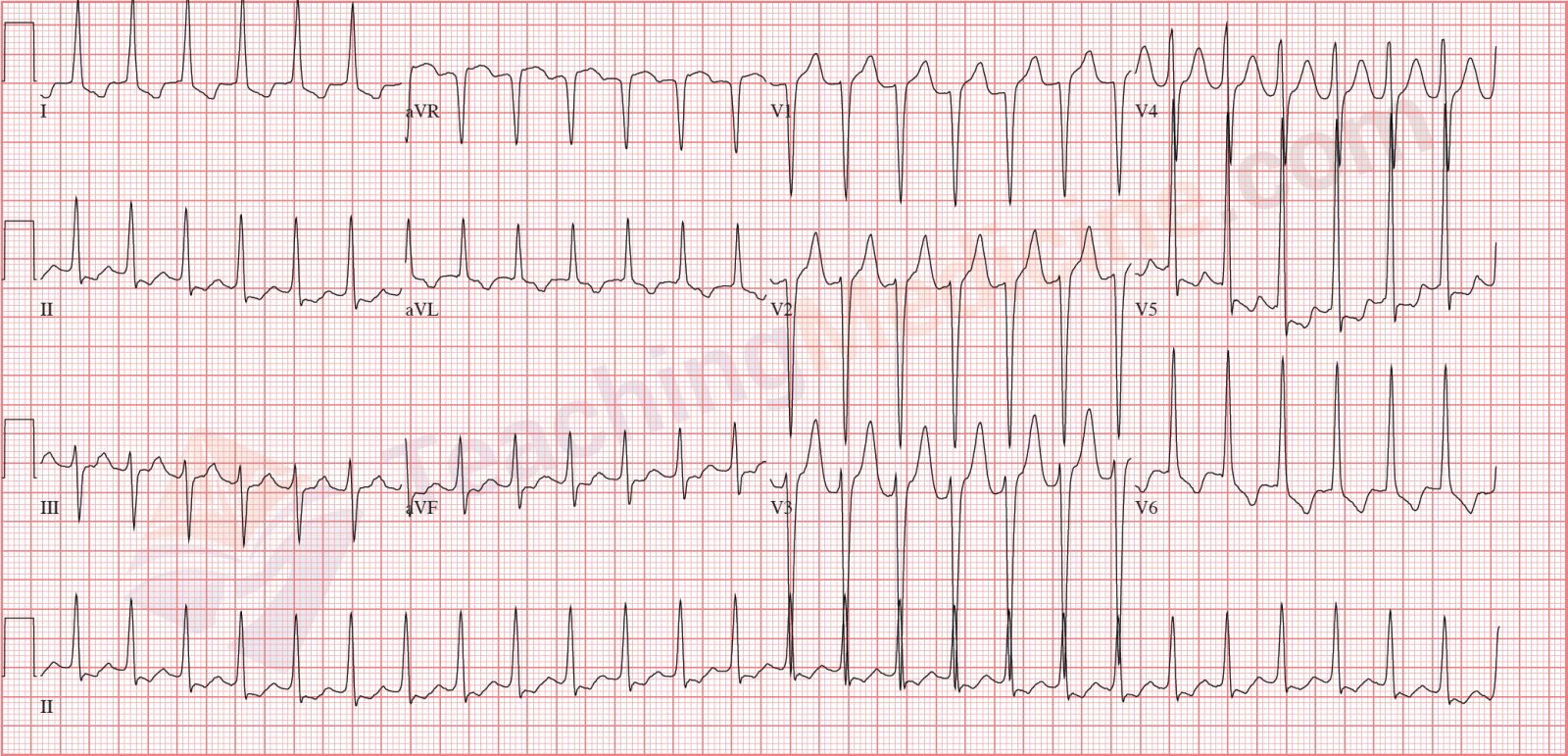
Examples: